Psoriasis
Understanding Psoriasis: A Comprehensive Guide
Psoriasis is a non-contagious skin condition caused by an abnormality in the immune system, leading to the increased production of new skin cells. Unable to shed old skin cells quickly enough, patients accumulate these dead cells on the skin’s surface, resulting in noticeable symptoms.Psoriasis presents itself in various types, such as:
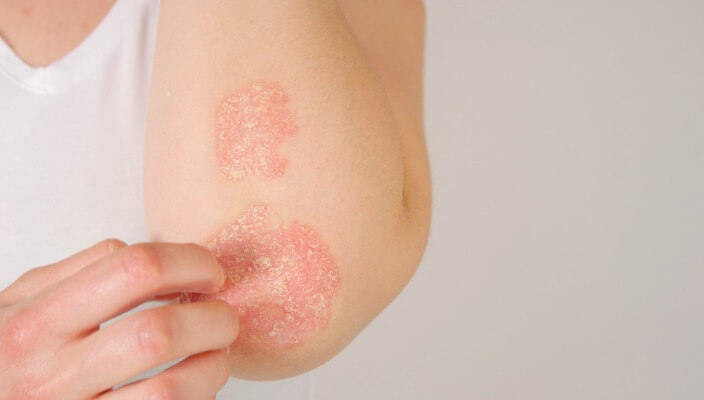
- Plaque psoriasis: The most common form of the disease. Presents itself as red and pink patches with silvery scale. Classic areas include the scalp, elbows, knees, hands and feet but can appear anywhere on the skin and can even affect the nails.
- Guttate psoriasis: This is the most common type of psoriasis diagnosed in children, but it can also present in adults. Sometimes the onset of guttate psoriasis follows a cold or flu like illness, such as strep throat.
- Pustular psoriasis: These are blistered, pus-filled lesions surrounded by reddened skin. Although it can appear anywhere, the hands and feet are often affected.
- Inverse psoriasis: Occurs in the areas of the body where the skin folds, such as the armpits and groin. Appears as smooth, inflamed red patches.
Managing Psoriasis Effectively
With proper dermatological care and guidance, you can manage your psoriasis and improve your skin health. Our goal is to help you achieve clearer, more comfortable skin through a comprehensive approach to treatment and care.
Start Your Journey to Healthier Skin
Don’t let psoriasis control your life. Schedule an appointment with a trusted provider at Westerville Dermatology and take the first step towards managing your condition effectively. With our expertise and commitment to your skin health, we are here to help you achieve and maintain healthy skin.
Examples of Psoriasis
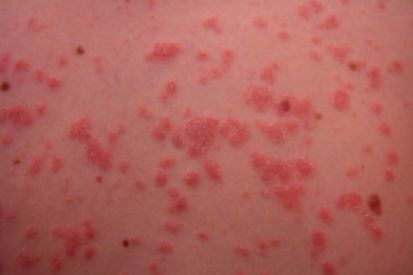
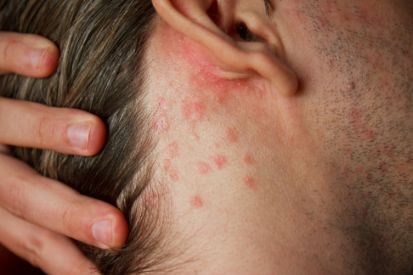
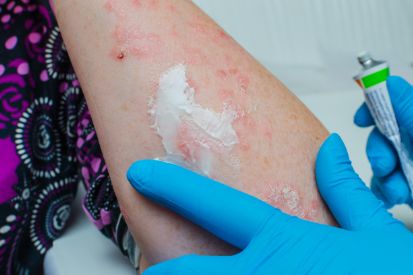
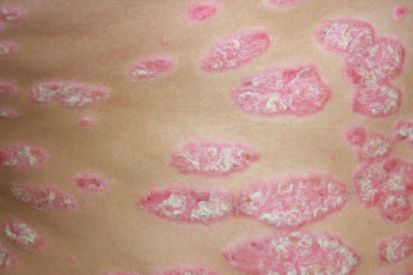
What are the Symptoms of Psoriasis?
- Red, inflamed skin.
- Silvery-white scales.
- Itching or burning sensation.
- Dry, cracked skin.
- Thickened or pitted nails.
- Joint pain and swelling in some cases.
What Causes Psoriasis?
- Genetic factors: Psoriasis often runs in families, suggesting a genetic predisposition to the condition.
- Immune system dysfunction: Abnormalities in the immune system can lead to an overactive response, triggering rapid skin cell growth.
- Other health conditions: Psoriasis is associated with an increased risk of other health issues such as cardiovascular disease, diabetes, and certain autoimmune disorders.
How to Prevent Psoriasis
Psoriasis FAQs
Psoriasis is a chronic condition, meaning it doesn't have a cure. However, it can be managed effectively with treatments and lifestyle adjustments. Many people with psoriasis lead healthy, fulfilling lives by finding the right approach to control flare-ups.
Weather can impact psoriasis, with some people experiencing flare-ups in certain conditions. Cold, dry weather can be harsh on the skin. Moisturizing regularly and adapting your skincare routine based on the weather can help minimize discomfort.
While it's generally possible, it's essential to take extra precautions. Psoriasis can affect how your skin reacts to tattoos, and flare-ups can complicate the healing process. Consulting with your dermatologist before getting a tattoo or piercing is advisable.
Stress is known to trigger or worsen psoriasis flare-ups. Finding effective stress management techniques, such as exercise, meditation, or hobbies, can be beneficial. Discussing stress management strategies with your healthcare team, including your dermatologist, can contribute to better psoriasis control.
No, psoriasis is not contagious. You can't "catch" it from someone else, and it's not something you can spread to others through contact. It's an immune system-related condition, not an infection.
From our QualDerm Family of Brands: Learn More About Psoriasis
Psoriasis Treatments
- Oral and injectable medications that affect the immune system to control the psoriasis.
- Tight therapy treatment.
- Laser treatment and more.
Our dermatologists tailor treatment plans to individual needs, emphasizing a balance between managing symptoms and minimizing potential side effects. Regular monitoring and follow-ups with our team of skin experts are crucial for effective psoriasis management and to develop a health skin routine for years to come.
Featured Blogs
- General Dermatology
- Chronic Skin Conditions
For the most part, psoriasis is managed with periodic dermatologic checkups and a lot of good home care. Because of its unique biological components, though, psoriasis may bring up additional reasons to call your dermatologist.
Read More
- General Dermatology
- Skin Care
- Chronic Skin Conditions
Hormonal acne can be a pesky skin problem for many. The only way to address this is by finding a hormonal acne treatment that works for you and your unique skin.
Read More
- Skin Cancer
- General Dermatology
- Chronic Skin Conditions
Learn more about the most common types of skin lesions we see at Westerville Dermatology and how our dermatologists remove them.
Read MoreFeatured Products

Avene Thermal Spring Water 5 oz
A naturally soothing source for sensitive skin since 1743, Avène Thermal Spring Water's unique composition is clinically shown by over 150 studies to calm, soothe and soften the skin. Ideal for red, sensitive or irritated skin and perfect for post-workout, travel, outdoor activities or to freshen up makeup.

Avene XeraCalm A.D Lipid Replenishing Balm 13.5 oz
Lipid-Replenishing Balm nourishes, soothes and calms dry, itchy skin prone to atopic dermatitis and eczema. Helps rebalance microbiome while supporting skin's defense system for a healthy skin. Safe for the entire family. 13.5 fl oz / 400 mL
