Skin Cancer
Understanding and Preventing Skin Cancer: Your Comprehensive Guide
Skin cancer is the most prevalent form of cancer globally. According to the Skin Cancer Foundation, 1 in 5 Americans will develop a form of skin cancer by the time they reach 70, highlighting the critical importance of awareness and prevention.
What is Skin Cancer?
Skin cancer occurs when abnormal cells grow uncontrollably in the skin. It often starts with changes in moles or new growths. The three most common forms of skin cancer are melanoma, basal cell carcinoma, and squamous cell carcinoma. Each type varies in severity and treatment approach, making early detection crucial.
Importance of Early Detection: Skin Cancer
Early detection is a key factor in the treatment of skin cancer, providing the best chance for favorable outcomes. Regular skin examinations by a dermatologist can help identify cancerous changes early. It is recommended to have a full body skin examination by a dermatologist annually to monitor for any suspicious changes or growths.
Benefits of Total Body Skin Exams
Total body skin exams allow our providers to analyze the overall health of your skin and check for any conditions or spots that may be of concern. This comprehensive approach ensures that any potential issues are caught early, allowing for prompt and effective treatment.
Our Commitment at Westerville Dermatology
At Westerville Dermatology, we’re dedicated to helping you achieve — and maintain — your skin’s best health through education, prevention, and the early detection of skin cancer. Our focus on skin health and positive outcomes is at the core of everything we do, which is why we offer a total body skin exam as part of your annual appointment.
Examples of Skin Cancer
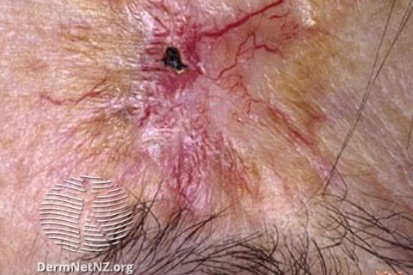
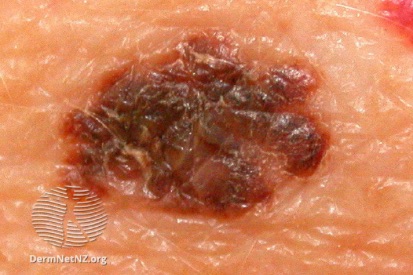
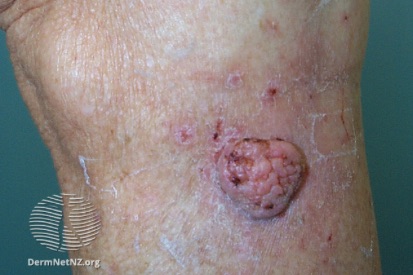
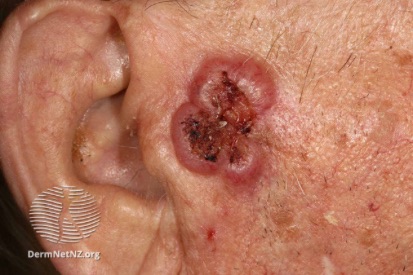

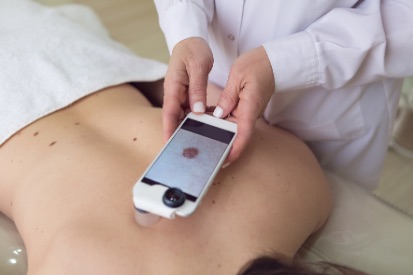
How to Spot Skin Cancer
Skin cancer can present in various ways, which is why it’s important to stay alert to any changes in your skin. Recognizing subtle or persistent skin changes early can significantly impact diagnosis and treatment outcomes for skin cancer. If you notice anything unusual, it’s best to consult a dermatologist at Pinnacle Dermatology for a professional evaluation.
Common skin cancer symptoms include:
- Changes in the size, shape, or color of existing moles
- New growths or spots that look different from other areas of your skin
- Sores or lesions that don’t heal, or heal and return
- Bumps that are pearly, waxy, or have a translucent appearance
- Rough, scaly patches or crusted areas on the skin
What Causes Skin Cancer?
As mentioned above, skin cancer often begins with damage to the DNA of skin cells, most commonly from ultraviolet radiation. Over time, this damage can lead to abnormal cell growth and cancer development.
At Pinnacle Dermatology, we understand the many factors contributing to skin cancer risk. We are committed to helping you identify and manage those risks through expert care, personalized prevention strategies, and routine skin exams.
Common skin cancer causes include:
- Excessive UV exposure from the sun or artificial sources like tanning beds
- Frequent sunburns, especially during childhood or adolescence
- Fair skin, light hair, and light-colored eyes (lower melanin levels mean less natural protection)
- A history of skin cancer or precancerous lesions
- Weakened immune system, due to illness or medications
- Exposure to toxic substances, such as arsenic
- Genetic factors or a family history of skin cancer
- Chronic skin inflammation or injuries in the same area over time
How to Prevent Skin Cancer
While skin cancer is one of the most common cancers, it’s also one of the most preventable. Every day presents an opportunity to protect your skin and reduce your risk through simple, consistent habits. From daily sun safety to staying aware of changes in your skin, skin cancer prevention starts with awareness—and ends with action.
At Pinnacle Dermatology, we empower our patients with the knowledge and care they need to take charge of their skin health. Through daily protection, self-checks, and annual total body skin exams, you can stay one step ahead and safeguard your health for the long term.
Daily Protection Habits
Daily protection starts with healthy skin habits. Use a broad-spectrum sunscreen with SPF 30 or higher every day, even on cloudy days, and reapply regularly. Wear protective clothing like wide-brimmed hats and long sleeves, and seek shade during peak sun hours (10 a.m. to 4 p.m.) to minimize UV exposure.
Importance of Regular Skin Self-Exams
Perform a monthly skin cancer self-exam to check for new moles or changes in existing spots. Use a mirror to examine all areas of your body, including hard-to-see places. If you notice anything suspicious, such as changes in shape, color, or size, schedule a visit with a dermatologist immediately.
Annual Total Body Skin Exams at Pinnacle Dermatology
An annual total body skin exam with a Pinnacle Dermatology provider offers a thorough, professional evaluation of your skin. During the exam, we check for any abnormal moles, lesions, or changes. Early detection dramatically improves treatment success, making these yearly exams vital to your skin health routine.
Skin Cancer FAQs
Skin cancer is a type of cancer that begins in the skin cells. It usually develops on skin exposed to the sun but can also occur in areas that are not exposed. There are three main types of skin cancer: basal cell carcinoma, squamous cell carcinoma, and melanoma. Basal cell carcinoma and squamous cell carcinoma are more common and have a higher cure rate, while melanoma is less common but more aggressive.
The primary risk factor for skin cancer is exposure to ultraviolet (UV) radiation from the sun or tanning beds. Other risk factors include having fair skin, a history of sunburns, a family history of skin cancer, a weakened immune system, and exposure to certain environmental factors such as arsenic.
The signs of skin cancer can vary depending on the type. Common signs include changes in the size, shape, color, or texture of a mole or spot on the skin. Itching, tenderness, or bleeding may also occur. It's crucial to be vigilant and seek medical attention if you notice any unusual changes on your skin.
Treatment for skin cancer depends on the type, size, and location of the cancer, as well as the patient's overall health. Common treatment options include surgical removal of the cancerous tissue, radiation therapy, and, in some cases, chemotherapy or immunotherapy. Early detection is key to successful treatment, so regular skin checks and prompt medical attention are crucial.
You should apply sunscreen every day, even on cloudy days and during the winter, UV rays can still penetrate the clouds and cause skin damage. Sunscreen needs time to be absorbed into the skin. We recommend applying it at least 15-30 minutes before going outdoors and reapplying every two hours.
A total body skin exam by a dermatologist is crucial for several reasons. Firstly, it serves as a proactive measure for the early detection of skin cancers, including melanoma, the deadliest form of skin cancer. Skin cancers are often highly treatable when identified at an early stage. A comprehensive examination allows the dermatologist to assess moles, birthmarks, and any unusual skin changes that may indicate potential issues.
Secondly, a dermatologist can identify and diagnose various skin conditions, including dermatitis, psoriasis, and infections. Early detection and treatment of these conditions can prevent them from escalating into more serious health issues.
Furthermore, a total body skin exam provides an opportunity to discuss and address any concerns or questions about skin health, sun protection, and skincare routines. Dermatologists can offer valuable guidance on skin cancer prevention, emphasizing the importance of sun protection measures, such as wearing sunscreen and protective clothing.
Regular skin exams become especially vital for individuals with risk factors, such as a family history of skin cancer, a personal history of sun exposure, or fair skin. Overall, a total body skin exam is a proactive and comprehensive approach to maintaining skin health, preventing skin cancers, and addressing any skin-related issues in a timely manner.
From our QualDerm Family of Brands: What to Expect at a Total Body Skin Exam
Skin Cancer Treatments
Receiving a skin cancer diagnosis can feel overwhelming, but treatment options today are highly effective, especially when the condition is caught early. At Pinnacle Dermatology, we provide personalized care plans tailored to your specific type, stage, and location of cancer. Whether your treatment involves non-surgical methods or advanced surgical techniques, our experienced providers are here to guide you every step of the way.
Non-Surgical Treatments
For certain types and early stages of skin cancer, non-surgical options can be effective. These may include topical medications, cryotherapy (freezing), or targeted therapies that destroy cancer cells without incisions. Your Pinnacle Dermatology provider will determine if a non-invasive approach is appropriate for your condition.
Surgical Treatments
Surgical treatments are often the most effective option for removing skin cancer, especially in more advanced or high-risk cases. Procedures may include excisional surgery or Mohs micrographic surgery, which precisely removes cancerous tissue while preserving healthy skin. Pinnacle Dermatology offers expert surgical care tailored to your needs and diagnosis.
Featured Blogs
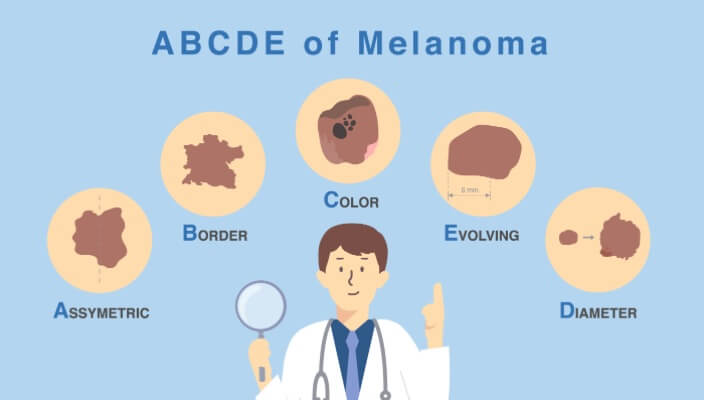
- Skin Cancer
- Skin Exams
Discover the ABCDEs of melanoma. Familiarize yourself with the five key indicators to aid in early detection and prompt medical attention for any suspicious moles or skin lesions.
Read More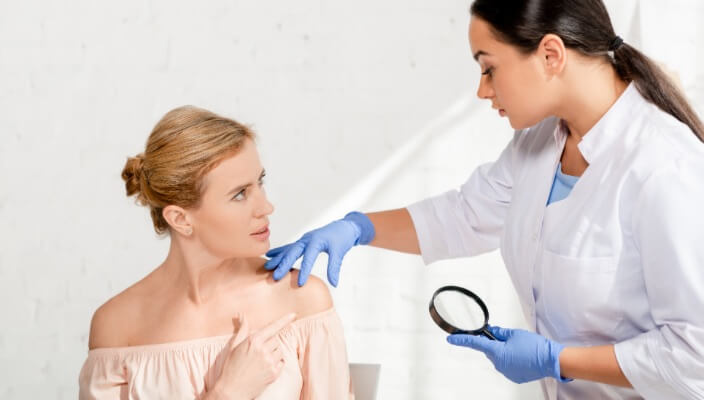
- Skin Cancer
- General Dermatology
- Skin Exams
- Sun Safety
If your dermatologist finds a suspicious mole during your TBSE, they want to perform a skin biopsy.
Read More
- Skin Cancer
- Skin Exams
In this blog, we’re covering what you need to know about five dangerous skin cancers, including basal cell carcinoma (BCC), squamous cell carcinoma (SCC), malignant melanoma, merkel cell carcinoma, and kaposi sarcoma.
Read MoreFeatured Products for Sun Protection

EltaMD UV Luminous Broad-Spectrum SPF 41
Get a shade more luminous with our newest lightly tinted sunscreen that brings skin care and essential sun care together. EltaMD UV Luminous Broad-Spectrum SPF 41 uses antioxidants such as linoleic acid and vitamin E to protect your skin from free radicals and diminish UV-related signs of aging. It’s light rosy tint and semi-matte finish blends into the skin seamlessly and blurs imperfections. EltaMD UV Luminous Broad-Spectrum SPF 41 sunscreen is ideal for those seeking non-greasy UV protection with all physical active ingredients. Net wt 1.7 oz/48 g

EltaMD UV Sheer Broad-Spectrum SPF 50
UV Sheer has a lightweight, hydrating formula that feels silky to the touch and light and airy on the skin. It goes on smooth absorbing quickly into skin and helps even out skin tone. This facial sunscreen offers up to 80 minutes of sweat and water-resistance making it the ideal choice for an active lifestyle, hot and humid weather and for anyone looking for a lightweight and hydrating sunscreen to live freely under the sun. UV Sheer is formulated to be compatible on all skin tones without leaving a white cast. 3.0 oz
